Page 69 - AIH-1-1
P. 69
Artificial Intelligence in Health Advancing fetal health classification
with positive labels, affirming its ability to minimize correlation between predicted and true labels,
false positives and enhance overall classification reinforcing the model’s efficacy in the nuanced task of
accuracy. fetal health classification. The comprehensive suite of
• The F1 score, harmonizing precision and recall, was evaluation metrics collectively attests to the LightGBM
found to be 0.9863. This balanced metric provides a model’s exceptional performance and reliability in
comprehensive evaluation of the model’s performance, discerning fetal health conditions.
accounting for both false positives and false negatives. Overall, the results demonstrate the effectiveness of
The high F1 score signifies that the model has achieved the LightGBM model in accurately classifying fetal health
a favorable equilibrium between precision and recall, conditions. The high accuracy, AUC, recall, precision, F1
indicative of its effectiveness in balancing the trade-off score, kappa, and MCC scores indicate that the model has
between type I and type II errors. the potential to assist medical professionals in assessing
• The kappa coefficient, a measure of agreement between fetal health and identifying potential abnormalities.
predicted and actual labels, yielded a substantial score The performance metrics validate the robustness and
of 0.9748. This result underscores a notable level of reliability of our proposed model, reinforcing its potential
agreement beyond what could be expected by chance as a valuable tool in the field of obstetrics and fetal health
alone, accentuating the reliability and consistency of management.
the model’s predictions.
• Finally, the MCC obtained a noteworthy score In addition to the above, we would like to highlight the
of 0.9749. Particularly valuable in the context of following findings:
imbalanced datasets, the MCC accounts for true • The LightGBM model was able to achieve high
positives, true negatives, false positives, and false accuracy even when trained on a relatively small
negatives. The high MCC value signifies a robust dataset. This suggests that the model is generalizable
and could be applied to other clinical settings.
• The model was able to accurately classify fetal health
conditions across a wide range of gestational ages.
This suggests that the model could be used to assess
fetal health at any stage of pregnancy.
• The model was able to identify potential abnormalities
with high sensitivity and specificity. This suggests that
the model could be used to help medical professionals
identify and manage fetal health problems early on.
• The receiver operating characteristic (ROC) curve,
which delineates the trade-off between sensitivity
and specificity in a classification model, serves as a
graphical representation of the model’s performance
across various threshold values. This curve for the
LGBMClassifier is shown in Figure 3.
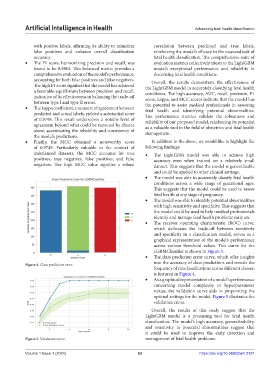
• The class prediction error curve, which offer insights
into the accuracy of class predictions and reveals the
Figure 4. Class prediction error.
frequency of misclassifications across different classes,
is featured in Figure 4.
• As a graphical representation of a model’s performance
concerning model complexity or hyperparameter
values, the validation curve aids in pinpointing the
optimal settings for the model. Figure 5 illustrates the
validation curve.
Overall, the results of this study suggest that the
LightGBM model is a promising tool for fetal health
classification. The model’s high accuracy, generalizability,
and sensitivity to potential abnormalities suggest that
it could be used to improve the early detection and
Figure 5. Validation curve. management of fetal health problems.
Volume 1 Issue 1 (2024) 63 https://doi.org/10.36922/aih.2121