Page 24 - GHES-2-2
P. 24
Global Health Econ Sustain Treatment and costs of skin lipohypertrophy
Table 2. Frequency of severe hypoglycemic events as well as related health and social costs in the control group and the intensive
education group
Event type Cost per Control group (n=318) Intervention group (n=395)
event (€) T‑6/T0 T0/T+6 T+6/T+12 T‑6/T0 T0/T+6 T+6/T+12
Events € Events € Events € Events € Events € Events €
(n=89) (n=72) (n=80) (n=91) (n=38) (n=12)
PHV 25.8 28 722.4 25 712.5 27 696.6 20 516 12 309.6 6 1548
ER 241.0 85 20485 83 20002 84 20.244 91 21931 40 9640 3 723
EMS 128.5 16 2056 15 1926.5 16 2.056 17 2184.5 14 1799 7 899.5
FM/CG WD 78.6 356 27981.6 333 25173.8 348 27.352,8 370 29082 116 9117.6 80 6120
DHC 750 24 18000 23 17.250 24 18.000 25 18750 14 10500 5 3750
Total cost (€) 69245 66064.8 68349.4 77107.5 20866.2 13045.5
∆% −4.6 −1.3 −72.9 −83.1
Note: The subjects in the control group have only been educated once in the beginning of insulin treatment. Source: Modified from Gentile et al. 2018a.
Abbreviations: PGV: Physician home visit; ER: Emergency room visit and treatment; EMS: Emergency medical services utilization/h; FM/CG WD:
Working days of a family member or caregiver (mean); DHC: Average daily hospitalization cost.
size of fatty cells. Buttocks, hips, abdomen, and limbs can
host LH nodules, thus requiring extensive intervention. In
this case, the attending surgeon needs to take the ability
of the skin to adapt to the new outlines of the body into
consideration, and such extensive intervention should only
be implemented on individuals with toned and elastic skin
to avoid poor aesthetic results and to remove the need for
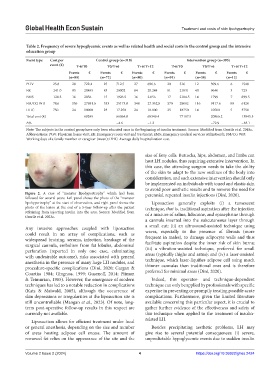
Figure 2. A case of “monster lipohypertrophy” which had been perennial, repeated insulin injections (Dini, 2020).
followed for several years. Left panel shows the photo of the “monster
lipohypertrophy” at the start of observation, and right panel shows the Liposuction generally exploits (i) a tumescent
photo of the lesion at the end of a 5-year follow-up after the patient technique, that is, traditional aspiration after the injection
refraining from injecting insulin into the area. Source: Modified from of a mixture of saline, lidocaine, and epinephrine through
Gentile et al. 2023a.
a cannula inserted into the subcutaneous layer through
a small cut; (ii) an ultrasound-assisted technique using
Any invasive approaches coupled with liposuction
could result in an array of complications, such as waves, especially in the presence of fibrosis (more
frequent in males), to damage adipocyte walls and thus
widespread bruising, seroma, infection, breakage of the facilitate aspiration despite the inner risk of skin burns;
surgical cannula, embolism from fat lobules, abdominal (iii) a vibration-assisted technique, preferred for small
perforation (reported in only one case, culminating
with undesirable outcome), risks associated with general areas (typically thighs and arms); and (iv) a laser-assisted
anesthesia in the presence of many large LH nodules, and technique, which laser-liquifies adipose cell using much
procedure-specific complications (Dini, 2020; Gargan & thinner cannulas than traditional ones and is therefore
Courtiss 1984; Gingrass, 1999; Gusenoff, 2014; Pitman preferred for minimal areas (Dini, 2020).
& Teimurian, 1985). However, the emergence of modern Indeed, this operator- and technique-dependent
techniques has led to a notable reduction in complications technique can only be applied by professionals with specific
(Katz & Maiwald, 2005), although the occurrence of expertise in preventing or promptly treating possible acute
skin depressions or irregularities at the liposuction site is complications. Furthermore, given the limited literature
still uncontrollable (Mangan et al., 2023). Of note, long- available concerning this particular aspect, it is crucial to
term post-operative follow-up results in this respect are gather further evidence of the effectiveness and safety of
currently not available. this technique when applied to the treatment of insulin-
Liposuction allows for efficient treatment under local related LH.
or general anesthesia, depending on the size and number Besides precipitating aesthetic problems, LH may
of areas hosting adipose cell excess. The amount of give rise to several potential consequences: (i) severe,
removed fat relies on the appearance of the site and the unpredictable hypoglycemic events due to sudden insulin
Volume 2 Issue 2 (2024) 4 https://doi.org/10.36922/ghes.2424