Page 24 - IJPS-8-2
P. 24
International Journal of
Population Studies Japan’s death-laden society
It is worth noting in this context that to date, the impact among most developed countries across the world (World
of the COVID-19 pandemic on this trend has remained Health Organization, 2008). Japan is no exception; as the
unclear. Japan first declared a state of emergency on world’s leading super-aged society, the country has been
April 7, 2020, following the World Health Organization’s contending with growing public health-care expenses for
declaration of a global pandemic on March 11, 2020. decades (Gilmour, Liao, Bilano, et al., 2014). This burden
According to the Ministry of Health, Labor and Welfare of disease is therefore the second area of challenge for
(2022), the figure was 71.3% as of March 2018, roughly Japan in its transition to a death-laden society, with the
2 years before the state of emergency, and 68.7% as of March financial costs projected to reach insolvency. This is the
2021, about a year after the first declaration of the state of case particularly if no major change is made to the way in
emergency. While no substantial change is observed during which people have conventionally relied on medical and
this period of time, one may argue, data of the coming few health-care resources during the last stage of their lives
years are necessary to make a more accurate projection of (Interview data, Nagoya, September 28, 2020).
the projected shortage in hospital beds.
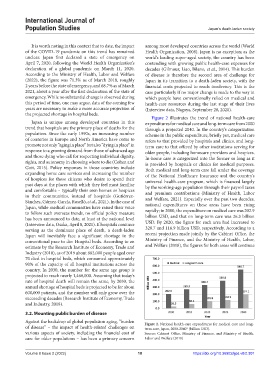
Figure 2 illustrates the trend of national health-care
Japan is unique among developed countries in this expenditures for medical care and long-term care from 2000
trend that hospitals are the primary place of deaths for the through a projected 2040. In the country’s categorization
population. Since the early 1990s, an increasing number scheme in the public expenditure, briefly put, medical care
of countries in Europe and North America have come to refers to that provided by hospitals and clinics, and long-
promote not only “aging in place” but also “dying in place” in term care to that offered by other institutions serving for
response to a growing demand from those of advanced age older people, including homecare providers and hospices.
and those dying who call for respecting individual dignity, In-home care is categorized into the former so long as it
rights, and autonomy in choosing where to die (Cohen and is provided by hospitals or clinics for medical purposes.
Gott, 2015). Policy responses in those countries include Both medical and long-term care fall under the coverage
expanding home care services and increasing the number of the National Healthcare Insurance and the country’s
of hospices for those citizens who desire to spend their universal health-care program, which is financed largely
past days at the places with which they feel most familiar by the working-age population through their payroll taxes
and comfortable – typically their own homes or hospices and premium contributions (Ministry of Health, Labor
in their communities, instead of hospitals (Gutiérrez- and Welfare, 2021). Especially over the past two decades,
Sánchez, Gómez-García, Roselló, et al., 2021). In the case of national expenditures on these areas have been rising
Japan, while medical communities have raised their voice
to follow such overseas trends, no official policy measure rapidly; in 2000, the expenditure on medical care was 202.9
has been announced to date, at least at the national level billion USD, and that on long-term care was 26.3 billion
(Interview data, Osaka, April 8, 2021). If hospitals continue USD. By 2020, the figure for each area had increased to
serving as the dominant place of death, a death-laden 328.7 and 116.9 billion USD, respectively. According to a
Japan will inevitably face a significant shortage in the recent projection made jointly by the Cabinet Office, the
conventional pace to die: Hospital beds. According to an Ministry of Finance, and the Ministry of Health, Labor,
estimate by the Research Institute of Economy, Trade and and Welfare (2018), the figures for both areas will continue
Industry (2018), as of 2019 about 882,000 people aged over
70 died in hospital beds, which consumed approximately
90% of the capacity of all hospital institutions across the
country. In 2030, the number for the same age group is
projected to reach nearly 1,460,000. Assuming that today’s
rate of hospital death will remain the same, by 2030, the
annual shortage of hospital beds is projected to be for about
600,000 patients, and the number will only grow over the
succeeding decades (Research Institute of Economy, Trade
and Industry, 2018).
3.2. Mounting public burden of disease
Against the backdrop of global population aging, “burden Figure 2. National health-care expenditures for medical care and long-
of disease” – the impact of health-related challenges on term care, Japan, 2000-2040* (billion USD).
various aspects of society, including the financial cost of Source: Cabinet Office, Ministry of Finance, and Ministry of Health,
care for older populations – has been a primary concern Labor and Welfare (2018)
Volume 8 Issue 2 (2022) 18 https://doi.org/10.36922/ijps.v8i2.301