Page 105 - BH-2-3
P. 105
Brain & Heart Adenosine cardiac arrest in aneurysm surgery
stable after 10 min of administration, although 13 patients
required vasoactive drugs. Bebawy et al. reported
5
23 patients who were given adenosine at 0.3 – 0.4 mg/kg
IV to facilitate temporary clipping of internal carotid artery
aneurysms with complex anatomical structures. Two
patients developed atrial fibrillation; otherwise, they were
hemodynamically stable. In another study, Guinn et al.
6
described 27 patients undergoing elective intracranial
aneurysm surgery in the anterior circulation, with adenosine
doses ranging from 3 to 60 mg IV. The study demonstrated
that AiCS effectively decompresses intracranial aneurysms
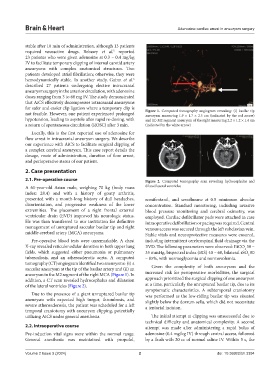
for safer and easier clip ligation where a temporary clip is Figure 1. Computed tomography angiogram revealing: (i) basilar tip
not feasible. However, one patient experienced prolonged aneurysm measuring 1.9 × 1.7 × 2.5 cm (indicated by the red arrow)
hypotension, leading to asystole after rapid re-dosing, with and (ii) M2 segment aneurysm of the right measuring 2.2 × 1.2 × 1.4 cm
a return of spontaneous circulation (ROSC) after 3 min. (indicated by the white arrow)
Locally, this is the first reported use of adenosine for
flow arrest in intracranial aneurysm surgery. We describe
our experience with AiCS to facilitate surgical clipping of
a complex cerebral aneurysm. This case report details the
dosage, route of administration, duration of flow arrest,
and perioperative status of our patient.
2. Case presentation
2.1. Pre-operative course Figure 2. Computed tomography scan revealing hydrocephalus and
A 61-year-old Asian male, weighing 70 kg (body mass dilated lateral ventricles
index: 28.4) and with a history of gouty arthritis,
presented with a month-long history of dull headaches, remifentanil, and sevoflurane at 0.5 minimum alveolar
disorientation, and progressive weakness of the lower concentration. Standard monitoring, including invasive
extremities. The placement of a right frontal external blood pressure monitoring and cerebral oximetry, was
ventricular drain (EVD) improved his neurologic status. employed. Cardiac defibrillator pads were attached in case
He was then transferred to our institution for definitive intraoperative defibrillation or pacing was required. Central
management of unruptured saccular basilar tip and right venous access was secured through the left subclavian vein.
middle cerebral artery (MCA) aneurysms. Stable vitals and neuroprotective measures were ensured,
Pre-operative blood tests were unremarkable. A chest including intermittent cerebrospinal fluid drainage via the
X-ray revealed reticulonodular densities in both upper lung EVD. The following parameters were observed: EtCO 30 –
2
fields, which suggested either pneumonia or pulmonary 35 mmHg, bispectral index (BIS) 40 – 60, bilateral rSO 80
2
tuberculosis, and an atherosclerotic aorta. A computed – 85%, with normoglycemia and normovolemia.
tomography (CT) angiogram identified two aneurysms: (i) a
saccular aneurysm at the tip of the basilar artery and (ii) an Given the complexity of both aneurysms and the
aneurysm in the M2 segment of the right MCA (Figure 1). In increased risk for perioperative morbidities, the surgical
addition, a CT scan revealed hydrocephalus and dilatation approach prioritized the surgical clipping of one aneurysm
of the lateral ventricles (Figure 2). at a time, particularly the unruptured basilar tip, due to its
symptomatic characteristics. A subtemporal craniotomy
Due to the presence of a giant unruptured basilar tip was performed as the low-riding basilar tip was situated
aneurysm with expected high turgor, thrombosis, and slightly below the dorsum sella, which did not necessitate
severe atherosclerosis, the patient was scheduled for a left a tentorial incision.
temporal craniotomy with aneurysm clipping, potentially
utilizing AiCS under general anesthesia. The initial attempt at clipping was unsuccessful due to
technical difficulty and anatomical complexity. A second
2.2. Intraoperative course attempt was made after administering a rapid bolus of
Pre-induction vital signs were within the normal range. adenosine (0.4 mg/kg IV) through central access, followed
General anesthesia was maintained with propofol, by a flush with 20 cc of normal saline IV. Within 5 s, the
Volume 2 Issue 3 (2024) 2 doi: 10.36922/bh.3394