Page 62 - IJPS-7-2
P. 62
International Journal of
Population Studies Child mortality by residence in Ethiopia
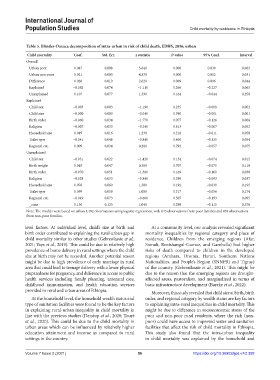
Table 5. Blinder‑Oaxaca decomposition of intra‑urban in risk of child death, EDHS, 2016, urban
Child mortality Coef. Std. Err. z statistic P‑value 95% Conf. Interval
Overall
Urban poor 0.047 0.008 5.640 0.000 0.030 0.063
Urban non-poor 0.021 0.005 4.330 0.000 0.012 0.031
Difference 0.026 0.010 2.620 0.009 0.006 0.044
Explained −0.082 0.074 −1.110 0.266 −0.227 0.063
Unexplained 0.107 0.077 1.390 0.164 −0.044 0.258
Explained
Child sex −0.003 0.003 −1.190 0.235 −0.008 0.002
Child size −0.000 0.000 −0.010 0.990 −0.001 0.001
Birth order −0.060 0.034 −1.770 0.077 −0.126 0.006
Religion −0.007 0.030 −0.240 0.813 −0.067 0.052
Household size 0.019 0.016 1.230 0.218 −0.011 0.050
Toilet type −0.041 0.048 −0.840 0.400 −0.135 0.054
Regional cat. 0.009 0.034 0.260 0.792 −0.057 0.075
Unexplained
Child sex −0.031 0.022 −1.420 0.154 −0.074 0.012
Birth weight 0.018 0.047 0.380 0.707 −0.075 0.110
Birth order −0.070 0.051 −1.380 0.169 −0.169 0.030
Religion −0.028 0.033 −0.840 0.399 −0.093 0.037
Household size 0.078 0.060 1.300 0.192 −0.039 0.195
Toilet type 0.059 0.059 1.000 0.317 −0.056 0.174
Regional cat. −0.049 0.073 −0.660 0.507 −0.193 0.095
_cons 0.130 0.125 1.040 0.298 −0.115 0.376
Note: The models were based on urban 1,482 observations using logistic regressions, with 643 observations from poor families and 839 observations
from non-poor families.
level factors. At individual level, child’s size at birth and At a community level, our analysis revealed significant
birth order contributed to explaining the rural-urban gap in mortality inequalities by regional category and place of
child mortality similar to other studies (Gebresilassie et al., residence. Children from the emerging regions (Afar,
2021; Yaya et al., 2019). This could be due to relatively high Somali, Benishangul-Gumuz, and Gambella) had higher
prevalence of home delivery in rural settings where the child risks of death compared to children in the developed
size at birth may not be recorded. Another potential reason regions (Amhara, Oromia, Harari, Southern Nations
might be due to high prevalence of early marriage in rural Nationalities, and People’s Region (SNNPR) and Tigray)
area that could lead to teenage delivery with a lower physical of the country (Gebresilassie et al., 2021). This might be
preparedness for pregnancy, and difference in access to public due to the reason that the emerging regions are drought-
health services including family planning, antenatal care, affected areas, pastoralists, and marginalized in terms of
childhood immunization, and health education services basic infrastructure development (Bareke et al., 2022).
provided in rural and urban areas of Ethiopia.
Moreover, this study revealed that child size at birth, birth
At the household level, the household wealth status and order, and regional category by wealth status are key factors
type of sanitation facilities were found to be the key factors to explaining intra-rural inequalities in child mortality. This
in explaining rural-urban inequality in child mortality in might be due to difference in socioeconomic status of the
line with the previous studies (Dendup et al., 2020; Touré poor and non-poor rural residents, where the rich (non-
et al., 2020). This could be due to the child mortality in poor) could have access to improved water and sanitation
urban areas which can be influenced by relatively higher facilities that affect the risk of child mortality in Ethiopia.
education attainment and income as compared to rural This study also found that the intra-urban inequality
settings in the country. in child mortality was explained by the household and
Volume 7 Issue 2 (2021) 56 https://doi.org/10.36922/ijps.v7i2.392