Page 20 - JCBP-2-2
P. 20
Journal of Clinical and
Basic Psychosomatics Allostatic overload in the medically ill
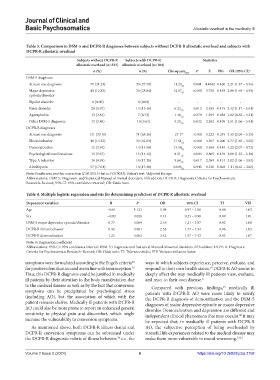
Table 3. Comparison in DSM‑5 and DCPR‑R diagnoses between subjects without DCPR‑R allostatic overload and subjects with
DCPR‑R allostatic overload
Subjects without DCPR‑R Subjects with DCPR‑R Statistics
allostatic overload (n=335) allostatic overload (n=104)
n (%) n (%) Chi‑square (df) P Z Phi OR (95% CI) a
DSM-5 diagnoses
At least one diagnosis 71 (21.25) 39 (37.50) 11.23 0.001 4.4042 0.160 2.21 (1.37 – 3.56)
(1)
Major depressive 43 (12.83) 30 (28.84) 14.67 (1) <0.001 3.758 0.183 2.89 (1.69 – 4.95)
episode/disorder
Bipolar disorder 0 (0.00) 0 (0.00) - - - - -
Panic disorder 20 (5.97) 14 (13.46) 6.23 (1) 0.013 2.485 0.119 2.42 (1.17 – 5.01)
Agoraphobia 13 (3.84) 7 (6.73) 1.48 (1) 0.279 1.295 0.058 1.62 (0.62 – 4.21)
Other DSM-5 diagnoses 13 (3.88) 10 (9.61) 5.25 0.022 2.282 0.109 2.51 (1.06 – 5.94)
(1)
DCPR-R diagnoses
At least one diagnosis 131 (39.10) 71 (68.26) 27.17 <0.001 5.223 0.249 3.35 (2.09 – 5.35)
Illness behavior 48 (14.32) 34 (32.69) 17.61 <0.001 4.107 0.200 2.77 (1.65 – 4.65)
(1)
Demoralization 12 (3.94) 14 (14.58) 13.58 (1) <0.001 3.486 0.184 4.22 (2.07 – 8.72)
Psychological manifestations 19 (5.67) 15 (14.42) 8.51 (1) 0.004 2.865 0.139 2.60 (1.25 – 5.38)
Type A behavior 30 (8.95) 18 (17.30) 5.68 0.017 2.389 0.114 2.02 (1.06 – 3.82)
(1)
Alexithymia 57 (17.01) 18 (17.30) 0.005 0.945 0.120 0.003 1.11 (0.61 – 202)
(1)
Note: Bonferroni post hoc correction (P≤0.05/15 that is P≤0.0033). Fisher’s test. Adjusted for age.
a
Abbreviations: DSM-5: Diagnostic and Statistical Manual of mental disorders, fifth edition; DCPR-R: Diagnostic Criteria for Psychosomatic
Research–Revised; 95% CI: 95% confidence interval; OR: Odds ratio.
Table 4. Multiple logistic regression analysis for determining predictors of DCPR‑R allostatic overload
Dependent variables B P OR 95% CI TI VIF
Age −0.01 1.121 0.98 0.97 – 1.00 0.96 1.03
Sex −0.82 0.026 0.44 0.21 – 0.90 0.99 1.01
DSM-5 major depressive episode/disorder 0.77 0.009 2.16 1.21 – 3.87 0.92 1.08
DCPR-R illness behavior 0.92 0.001 2.53 1.47 – 4.34 0.96 1.03
DCPR-R demoralization 1.23 0.002 3.42 1.57 – 7.43 0.93 1.07
Note: B: Regression coefficient
Abbreviations: 95% CI: 95% confidence interval; DSM-5: Diagnostic and Statistical Manual of mental disorders, fifth edition; DCPR-R: Diagnostic
Criteria for Psychosomatic Research–Revised; OR: Odds ratio; TI: Tolerance index; VIF: Variance inflation factor.
symptoms were formulated according to the Engel’s criteria ways in which subjects experience, perceive, evaluate, and
38
for positive identification and are in line with interoception. respond to their own health status. DCPR-R AO seems to
39
10
Thus, this DCPR-R diagnosis could be justified in medically deeply affect the way medically ill patients view, evaluate,
ill patients by their attention to the body manifestation due and react to their own disease. 6
to the medical disease as well as by the fact that conversion Compared with previous findings, medically ill
15
symptoms can be precipitated by psychological stress patients with DCPR-R AO were more likely to satisfy
(including AO), but the association of which with the the DCPR-R diagnosis of demoralization and the DSM-5
patient remains elusive. Medically ill patients with DCPR-R diagnoses of major depressive episode or major depressive
AO could also be more prone to report an enhanced general disorder. Demoralization and depression are different and
sensitivity to physical pain and discomfort, which might independent clinical phenomena that may coexist. It may
40
increase the vulnerability to conversion symptoms. be expected that, in medically ill patients with DCPR-R
As mentioned above, both DCPR-R illness denial and AO, the subjective perception of being overloaded by
DCPR-R conversion symptoms can be subsumed under stressful life experiences related to the medical disease may
the DCPR-R diagnostic rubric of illness behavior, i.e., the make them more vulnerable to mood worsening. 12,15
10
Volume 2 Issue 2 (2024) 6 https://doi.org/10.36922/jcbp.2758