Page 41 - JCBP-3-1
P. 41
Journal of Clinical and
Basic Psychosomatics Psychosomatic influences on insomnia
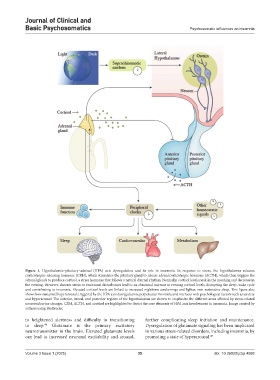
Figure 1. Hypothalamic–pituitary–adrenal (HPA) axis dysregulation and its role in insomnia. In response to stress, the hypothalamus releases
corticotropin-releasing hormone (CRH), which stimulates the pituitary gland to release adrenocorticotropic hormone (ACTH), which then triggers the
adrenal glands to produce cortisol, a stress hormone that follows a natural diurnal rhythm. Normally, cortisol levels peak in the morning and decrease in
the evening. However, chronic stress or emotional disturbances lead to an abnormal increase in evening cortisol levels, disrupting the sleep–wake cycle
and contributing to insomnia. Elevated cortisol levels are linked to increased nighttime awakenings and lighter, non-restorative sleep. This figure also
shows how sustained hyperarousal, triggered by the HPA axis dysregulation, perpetuates insomnia and interacts with psychological factors such as anxiety
and hyperarousal. The anterior, lateral, and posterior regions of the hypothalamus are shown to emphasize the different areas affected by stress-related
neuroendocrine changes. CRH, ACTH, and cortisol are highlighted to depict the core elements of HPA axis involvement in insomnia. Image created by
authors using BioRender.
to heightened alertness and difficulty in transitioning further complicating sleep initiation and maintenance.
to sleep. Glutamate is the primary excitatory Dysregulation of glutamate signaling has been implicated
48
neurotransmitter in the brain. Elevated glutamate levels in various stress-related disorders, including insomnia, by
can lead to increased neuronal excitability and arousal, promoting a state of hyperarousal. 49
Volume 3 Issue 1 (2025) 35 doi: 10.36922/jcbp.4588