Page 98 - JCBP-3-1
P. 98
Journal of Clinical and
Basic Psychosomatics Functional neurological movement disorders
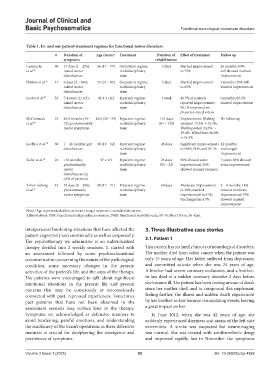
Table 1. In- and out-patient treatment regimes for functional motor disorders
n Duration of Age (years) a Treatment Duration of Effect of treatment Follow up
symptoms rehabilitation
Czarnecki 60 17 days (1 – 276); 46 (17 – 79) Outpatient regime; 5 days Marked improvement 25 months; 60%
et al. 26 mixed motor multidisciplinary in 75% still showed marked
disturbances team improvement
Nielsen et al. 25 47 6 days (2 – 480); 44 (21 – 85) Outpatient regime; 5 days Marked improvement 3 months; 55% still
mixed motor multidisciplinary in 65% showed improvement
disturbances team
Jacobs et al. 27 32 7.4 years (±10.3); 49.1 ± 14.2 Inpatient regime; 1 week 86.7% of patients 6 months; 69.2%
mixed motor multidisciplinary reported improvement; showed improvement
disturbances team 59.1% improved on
physician-rated videos
McCormack 33 48.8 months (19 – 40.8 (20 – 59) Inpatient regime; 101 days Improvement: Walking No follow up
et al. 29 72); predominantly multidisciplinary (84 – 130) unaided: 15.2% → 42.4%;
motor symptoms team Walking aided: 24.2% →
39.4%; Wheelchair: 60.6%
→ 18.2%
Jordbru et al. 28 60 1 – 48 months; gait 38 (19 – 62) Inpatient regime; 28 days Significant improvements 12 months;
disturbances multidisciplinary in FMS, FIM, and SF-36 unchanged
team improvement
Saifee et al. 30 26 >36 months; 47 ± 9.5 Inpatient regime; 24 days 58% showed some 7 years; 58% showed
predominantly multidisciplinary (15 – 32) improvement; 35% some improvement
motor team showed no improvement
disturbances (in
63% of patients)
Arlien-Søborg 42 53 days (0 – 240); 39 (17 – 71) Inpatient regime; 60 days Moderate improvement 3 – 6 months; 14%
et al. 31 predominantly multidisciplinary in 28%; marked showed moderate
motor symptoms team improvement in 67%; improvement; 79%
Unchanged in 4.7% showed marked
improvement
Note: Age is presented either as mean (range) or mean ± standard deviation.
a
Abbreviations: FIM: Functional independence measure; FMS: Functional mobility scale; SF-36: Short Form, 36-item.
interpersonal burdening situations that have affected the 3. Three illustrative case stories
patient cognitively and emotionally as well as corporeally.
The psychotherapy we administer is an individualized 3.1. Patient 1
therapy divided into 2 weekly sessions. It started with This patient has no family history of neurological disorders.
an assessment followed by some psychoeducational Her mother died from colon cancer when the patient was
communication concerning the nature of the pathological only 15 years of age. Her father suffered from depression
condition, some necessary changes in the present and committed suicide when she was 24 years of age.
activities of the patient’s life, and the aims of the therapy. A brother had severe coronary occlusions, and a brother-
The patients were encouraged to talk about significant in-law died of a sudden coronary disorder 2 days before
emotional situations in the present life and present she became ill. The patient has been feeling unease of death
patterns that may be consciously or unconsciously since her mother died, and to compound this unpleasant
connected with past, repressed experiences. Sometimes feeling further, the illness and sudden death experienced
past patterns that have not been observed in the by her brother-in-law became traumatizing events, leaving
assessment sessions may surface later in the therapy. a great impact on her.
Symptoms are acknowledged as defensive manners to In June 2012, when she was 42 years of age, she
avoid burdening, painful emotions, and understanding suddenly experienced dizziness and ataxia of the left-side
the machinery of the brain’s operations in these defensive extremities. A stroke was suspected but neuroimaging
manners is crucial for deciphering the emergence and was normal. She was treated with antithrombotic drugs
persistence of symptoms. and improved rapidly, but in November the symptoms
Volume 3 Issue 1 (2025) 92 doi: 10.36922/jcbp.4369