Page 10 - AIH-2-2
P. 10
Artificial Intelligence in Health Role of LLMs in improving patient experience
Table 1. Inclusion and exclusion criteria
Criteria Inclusion criteria Exclusion criteria
Study type Prospective studies, cross-sectional studies, and systematic Studies focusing on non-LLM AI models or other machine
reviews that discuss the applications of LLMs in patient learning techniques unrelated to patient experience.
satisfaction, communication, or experience. Studies employing LLMs solely for generating manuscripts or
text without any commentary on patient outcomes.
Date range Articles published between January 2015 and June 2024. Articles published before January 2015
Language Articles published in English. Articles published in languages other than English
Study focus Research discussing LLMs applied in healthcare settings, Studies focusing on administrative tasks without discussing the
enhancing communication, education, or experience. patient-facing impact or satisfaction.
Outcome measures Studies evaluating outcomes such as patient satisfaction, Studies lacking specific outcome measures related to patient
communication improvement, or operational efficiency. experience or satisfaction.
Comparator Studies comparing LLM interventions with traditional Studies with no comparator group or irrelevant comparisons.
methods (e.g., human communication or standard protocols).
Abbreviations: LLM: Large language model; AI: Artificial intelligence.
Thailand, 1 Italy, 1 through accurate or faster diagnosis or through superior
Netherlands, 1 Japan, 1 patient communication channels) or indirect means (e.g.,
Singapore, 1
Israel, 1 through improved operational efficiency resulting in
Canada, 1 reduced waiting times). Both are of value, although the
Saudi Arabia, significance to the patient is more evident in the former. In
2
general, the following areas were examined:
China, 3 • Answering patient queries: Given the readily prompted
USA, 24 patient-facing interface of ChatGPT, the immediate
Germany, 4
interest was in the possibility of training LLMs to
address a patient’s specific health-related questions
India, 4 in a broad or specific context. Eight articles have
investigated this, ranging from questions on general
23
UK, 3 health to specific areas such as cirrhosis and
hepatocellular carcinoma, total hip arthroplasty,
24
25
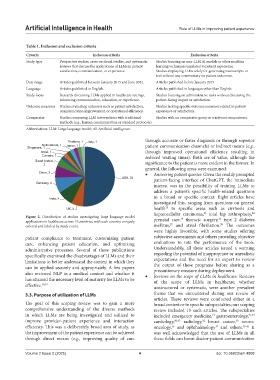
Figure 2. Distribution of studies investigating large language model 29 26
applications in healthcare across 13 countries, with each country uniquely prenatal care, thoracic surgery, type 2 diabetes
28
27
colored and labeled by study count. mellitus, and atrial fibrillation. The outcomes
were highly favorable, with some studies offering
patient compliance to treatment, customizing patient subjective assessments and others providing objective
care, enhancing patient education, and optimizing evaluations to rate the performance of the tools.
administrative processes. Several of these publications Understandably, all these articles issued a warning
specifically examined the disadvantages of LLMs and their regarding the potential of inappropriate or unrealistic
limitations to better understand the context in which they expectations and the need for an expert to review
the output of these programs before sharing as a
can be applied securely and appropriately. A few papers precautionary measure during deployment.
also reviewed NLP in a medical context and whether it • Reviews on the scope of LLMs in healthcare: Reviews
has attained the necessary level of maturity for LLMs to be of the scope of LLMs in healthcare, whether
effective. 18,19 unstructured or systematic, were another prevalent
3.3. Purpose of utilization of LLMs theme that we encountered during our review of
articles. These reviews were conducted either in a
The goal of this scoping review was to gain a more broad context or in specific subspecialties; our scoping
comprehensive understanding of the diverse methods review included 15 such articles. The subspecialties
in which LLMs are being investigated and utilized to included emergency medicine, gastroenterology, 31,34
19
improve provider–patient experience and interaction cardiology, 30,35 radiology, breast cancer, neuro-
33
32
efficiency. This was a deliberately broad area of study, as oncology, and ophthalmology and others. 38-41 It
37
36
the improvement of the patient experience can be achieved was well acknowledged that the use of LLMs in all
through direct means (e.g., improving quality of care these fields can boost doctor-patient communication
Volume 2 Issue 2 (2025) 4 doi: 10.36922/aih.4808