Page 46 - AN-2-2
P. 46
Advanced Neurology Seizures and CKD
Dialysis‑related dose adjustments US: Advised to avoid given insufficient data to support use at present UK: Drug not included in the RDH US: 50% dosing supplementation likely needed per post-dialysis session UK: No dose adjustments needed US: No dose adjustments needed UK: No dose adjustments needed US: 50% supplemental dosing needed post-HD UK: Give 25% of the patient normal dose for patients receiving HD and titrating
(mL/min/1.73 m 2 ) reduction advised for eGFR < 60 and to prescribe with caution with close included in the RDH reduction with eGFR < 30 with regular serum level adjustments needed adjustments needed adjustments needed reduction with eGFR 30 – 59. 50% dose reduction with eGFR 1529. 75% dose reduction with eGFR UK: Give 75% of normal dose for eGFR 50–80. Give 50% of normal dose for 25% of normal dose when eGFR < 3
eGFR related dose adjustments US: 50% dose monitoring. UK: Drug not US: 50% dose monitoring UK: No dose US: No dose UK: No dose US: 25% dose < 15 response.
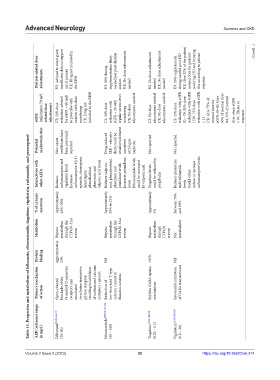
Table 15. Properties and metabolism of felbamate, ethosuximide, tiagabine, vigabatrin, rufinamide, and perampanel
Potential nephrotoxicities New-onset urolithiasis have been previously reported Drug-induced SLE – whereby there could be renal involvement consistent with lupus nephritis Not reported Not reported
Interactions with other AEDs Reduces carbamazepine and vigabatrin levels Increases carbamazepine-10,11 epoxide, clonazepam, lamotrigine, phenobarbital, phenytoin and valproic acid levels Reduces valproic acid, phenobarbital, phenytoin and primidone levels Increases primidone levels Ethosuximide levels could be increased by valproic acid Tiagabine levels could be reduced by pregabalin Reduces phenytoin and rufina
% of urinary excretion Approximately 40%–50% Approximately 20% to 25% Approximately 1% Between 70% and 80%
Metabolism Hepatic metabolism through the CYP450-3A4 system Hepatic metabolism through the CYP450-3A4 system Hepatic metabolism through CYP450 system Not metabolized
Protein binding Approximately 25% Nil >95% Nil
Primary mechanism of action Open-channel blockade of the N-methyl-D-aspartate receptors and associated strychnine-insensitive glycine receptor, resulting in inhibition of sodium and calcium excitatory currents Reduction of low-threshold T-type calcium current in thalamic neurons Inhibits GABA uptake mechanism Irreversible inhibition of GABA transaminase
AED (reference range in mg/L) Felbamate [9,129,169-171] (30–60) Ethosuximide [130,131,172-174] (40 – 100) Tiagabine [9,129,130,175] (0.02 – 0.2) Vigabatrin [9,129,130,176] (0.8 – 36)
20
https://doi.org/10.36922/an.314
Volume 2 Issue 2 (2023) olume 2 Issue 2 (2023)
V 20 https://doi.org/10.36922/an.314