Page 133 - AN-3-3
P. 133
Advanced Neurology Delayed occlusion after mechanical thrombectomy
significant medical history and was not on any medication. after admission. During outpatient follow-ups with
Neurological examination showed mild left facial paresis regular MRI scans, a follow-up MRI at 3-month post-
and left upper limb weakness. His National Institutes onset revealed no ischemic lesion but showed occlusion
of Health Stroke Scale score was 2 points at admission, of the right MCA compared to the MRI at 1-month post-
and his symptoms were unstable. An emergent magnetic onset (Figure 2A: Immediate post-onset; Figure 2B: One-
resonance imaging (MRI) revealed no apparent diffusion- month post-onset; Figure 2C: Three-month post-onset).
weighted imaging-positive lesions (Figure 1A and B) but The patient was readmitted to evaluate the occlusion
showed an occlusion in the proximal portion of the right status and cerebral blood flow. Cerebral angiography
middle cerebral artery (MCA) (Figure 1C). Intravenous demonstrated filling of the distal MCA territory through
administration of tissue plasminogen activator (tPA) collateral pathways (Figure 2D). Acetazolamide-
was followed by MT using the direct aspiration first pass challenged single-photon emission computed tomography
technique (ADAPT). This procedure achieved reperfusion revealed reduced resting cerebral blood flow and impaired
6
with thrombolysis in cerebral infarction grade 3 score, cerebrovascular reactivity in the right MCA territory
3 h and 46 min after symptom onset (Figure 1D and E). (Figure 2E). After a thorough discussion with the patient
Subsequent three-dimensional rotational angiography and family, an EC-IC bypass surgery was performed for
revealed residual stenosis of approximately 70% based on stroke prevention (Figure 3A-C). The patient continued
the Warfarin–Aspirin Symptomatic Intracranial Disease dual antiplatelet therapy and statin treatment until the
criteria (Figure 1F). This finding prompted the initiation surgery. Postoperatively, no new neurological deficits
of dual antiplatelet therapy with clopidogrel 75 mg (Nichi- were observed, and MRI revealed patent bypass arteries
Iko, Japan) and aspirin 100 mg (Bayer, Japan) daily. Due with improved signal intensity in the peripheral MCA
to mild dyslipidemia identified in the blood test results at branches. Subsequently, the patient transitioned from dual
admission, rosuvastatin 5 mg (Sanwa Kagaku Kenkyusho, antiplatelet therapy to a single agent. Three-month post-
Japan) was also started and continued. surgery, the modified Rankin Scale indicated no disability
As there were no recurrent symptoms or evidence of (score of 0), and the patient resumed work without
reocclusion, the patient was discharged on the 18 day experiencing any new ischemic episodes.
th
A B D E
C
F
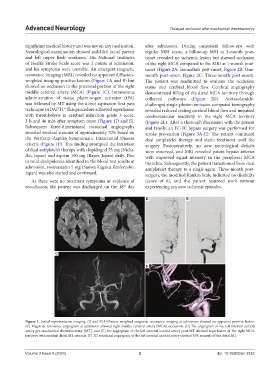
Figure 1. Initial representative imaging. (A and B) Diffusion-weighted magnetic resonance imaging at admission showed no apparent positive lesion.
(C) Magnetic resonance angiogram at admission showed right middle cerebral artery (MCA) occlusion. (D) The angiogram of the left internal carotid
artery pre-mechanical thrombectomy (MT), and (E) the angiogram of the left internal carotid artery post-MT showed reperfusion of the right MCA
territory with residual distal M1 stenosis. (F) 3D rotational angiogram of the left internal carotid artery showed 70% stenosis of the distal M1.
Volume 3 Issue 3 (2024) 2 doi: 10.36922/an.3332