Page 15 - ARNM-1-1
P. 15
Advances in Radiotherapy
& Nuclear Medicine Seed implantation head-and-neck carcinoma
A B or the skull base. The prescribed dose was 100 – 160 Gy.
The 2-, 5-, and 10-year LC rates were 86.3%, 59%, and
31.5%, respectively. The 2-, 5-, and 10-year OS rates were
92.1%, 65%, and 34.1%, respectively. Tumors >6 cm had
significantly lowered LC and OS. No severe complications
were observed during the follow-up period. I-125 RSI-BT
is a feasible and effective modality for the treatment of
C locally advanced unresectable or recurrent ACC.
Mao et al. conducted a study involving 24 patients
[22]
diagnosed with mucoepidermoid carcinoma (MEC)
of the parotid gland. Patients with high-risk factors
underwent I-125 RSI-BT (median actuarial D90: 97 Gy)
within 4 weeks following surgery. The radioactivity
administered ranged from 18.5 to 33.3 MBq per seed, and
the PD ranged from 60 to 120 Gy. The follow-up period
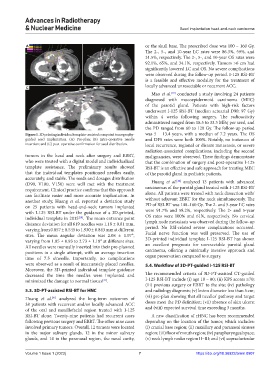
Figure 1. 3D printing individual template-assisted computed tomography- was 5 – 13.4 years, with a median of 7.2 years. The OS
guided seed implantation. (A) Pre-plan; (B) intra-operative needle and DFS rates were both 100%. Notably, no instances of
insertion; and (C) post-operative confirmation for seed distribution. local recurrence, regional or distant metastasis, or severe
radiation-associated complications, including the second
tumors in the head and neck after surgery and EBRT, malignancies, were observed. These findings demonstrate
who were treated with a digital model and individualized that the combination of surgery and post-operative I-125
template assistance. The preliminary results showed RSI-BT is an effective and safe approach for treating MEC
that the individual templates positioned needles easily, of the parotid gland in pediatric patients.
accurately, and stable. The seeds and dosages distribution [42]
(D90, V100, V150) were well met with the treatment Huang et al. analyzed 13 patients with advanced
requirement. Clinical practice confirms that this approach carcinomas of the parotid gland treated with I-125 RSI-BT
can facilitate easier and more accurate implantation. In alone. All patients were treated with neck dissection with/
another study, Huang et al. reported a deviation study without adjuvant EBRT for the neck simultaneously. The
on 25 patients with head-and-neck tumors implanted PD of RSI-BT was 140–160 Gy. The 2- and 5-year LC rates
with I-125 RSI-BT under the guidance of a 3D-printed, were 91.7% and 58.2%, respectively. The 2- and 5-year
individual template in 2015 . The mean entrance point OS rates were 100% and 61%, respectively. No cervical
[18]
distance deviation for all 619 needles was 1.18 ± 0.81 mm, lymph node metastasis was observed during the follow-up
varying from 0.857 ± 0.545 to 1.930 ± 0.843 mm at different period. No RSI-related severe complications occurred.
sites. The mean angular deviation was 2.08 ± 1.07°, Facial nerve function was well preserved. The use of
varying from 1.85 ± 0.93 to 2.73 ± 1.18° at different sites. 3D-printed individual template I-125 RSI-BT has shown
All needles were manually inserted into their pre-planned an excellent prognosis for unresectable parotid gland
positions in a single attempt, with an average insertion carcinoma, offering a minimally invasive approach and
time of 7.5 s/needle. Importantly, no complications organ preservation compared to surgery.
were observed as a result of inaccurately placed needles. 5.4. Workflow of 3D-PT-guided I-125 RSI-BT
Moreover, the 3D-printed individual template guidance
decreased the time the needles were implanted and The recommended criteria of 3D-PT-assisted CT-guided
minimized the damage to normal tissues . I-125 RSI-BT include (i) age 18 – 80; (ii) KPS scores ≥70;
[41]
(iii) previous surgery or EBRT to the site; (iv) pathology
5.3. 3D-PT-assisted RSI-BT for HNC and radiology diagnosis; (v) lesion diameter less than 5 cm;
Huang et al. analyzed the long-term outcomes of (vi) pre-plan showing that all needles’ pathway and target
[41]
38 patients with recurrent and/or locally advanced ACC doses meet the PD definition; (vii) absence of skin ulcers;
of the oral and maxillofacial region treated with I-125 and (viii) expected survival time exceeding 3 months.
RSI-BT alone. Twenty-nine patients had recurrent cases A new classification of rHNC has been recommended
following previous surgery and EBRT. The other nine cases depending on the location of the tumor, which includes:
involved primary tumors. Overall, 12 tumors were located (i) cranial base region; (ii) maxillary and paranasal sinuses
in the major salivary glands, 12 in the minor salivary region; (iii) floor of mouth region; (iv) parapharyngeal space;
glands, and 14 in the paranasal region, the nasal cavity, (v) neck lymph nodes region Ⅱ–Ⅲ; and (vi) supraclavicular
Volume 1 Issue 1 (2023) 7 https://doi.org/10.36922/arnm.0907