Page 76 - ARNM-2-2
P. 76
Advances in Radiotherapy
& Nuclear Medicine Wound reconstruction with Intergra®
A B C
D E F
G H I
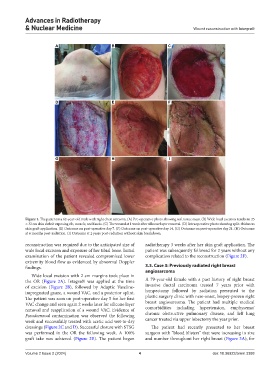
Figure 1. The patient is a 62-year-old male with right chest sarcoma. (A) Pre-operative photo showing soft tissue mass. (B) Wide local excision results in 25
× 32 cm skin deficit exposing rib, muscle, and fascia. (C) The wound at 1 week after silicone layer removal. (D) Intraoperative photo showing split-thickness
skin graft application. (E) Outcome on post-operative day 7. (F) Outcome on post-operative day 14. (G) Outcome on post-operative day 21. (H) Outcome
at 6 months post-radiation. (I) Outcome at 2 years post-radiation without skin breakdown.
reconstruction was required due to the anticipated size of radiotherapy 3 weeks after her skin graft application. The
wide local excision and exposure of her tibial bone. Initial patient was subsequently followed for 2 years without any
examination of the patient revealed compromised lower complication related to the reconstruction (Figure 2F).
extremity blood flow as evidenced by abnormal Doppler
findings. 3.3. Case 3: Previously radiated right breast
angiosarcoma
Wide local excision with 2 cm margins took place in
the OR (Figure 2A). Integra® was applied at the time A 79-year-old female with a past history of right breast
of excision (Figure 2B), followed by Adaptic Vaseline- invasive ductal carcinoma treated 7 years prior with
impregnated gauze, a wound VAC, and a posterior splint. lumpectomy followed by radiation presented to the
The patient was seen on post-operative day 5 for her first plastic surgery clinic with new-onset, biopsy-proven right
VAC change and seen again 2 weeks later for silicone layer breast angiosarcoma. The patient had multiple medical
removal and reapplication of a wound VAC. Evidence of comorbidities including hypertension, emphysema/
Pseudomonal contamination was observed the following chronic obstructive pulmonary disease, and left lung
week and successfully treated with acetic acid wet-to-dry cancer treated via upper lobectomy the year prior.
dressings (Figure 2C and D). Successful closure with STSG The patient had recently presented to her breast
was performed in the OR the following week. A 100% surgeon with “blood blisters” that were increasing in size
graft take was achieved (Figure 2E). The patient began and number throughout her right breast (Figure 3A), for
Volume 2 Issue 2 (2024) 4 doi: 10.36922/arnm.3388