Page 50 - BH-2-3
P. 50
Brain & Heart Balloon valvuloplasty for aortic stenosis
A B
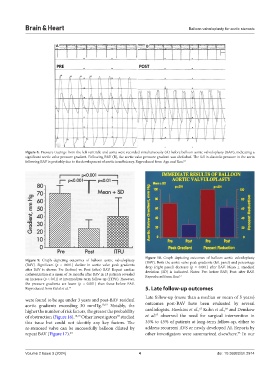
Figure 8. Pressure tracings from the left ventricle and aorta were recorded simultaneously (A) before balloon aortic valvuloplasty (BAV), indicating a
significant aortic valve pressure gradient. Following BAV (B), the aortic valve pressure gradient was abolished. The fall in diastolic pressure in the aorta
following BAV is probably due to the development of aortic insufficiency. Reproduced from Agu and Rao. 12
Figure 10. Graph depicting outcomes of balloon aortic valvuloplasty
Figure 9. Graph depicting outcomes of balloon aortic valvuloplasty (BAV). Both the aortic valve peak gradients (left panel) and percentage
(BAV). Significant (p < 0.001) decline in aortic valve peak gradients drop (right panel) decrease (p = 0.001) after BAV. Mean ± standard
after BAV is shown: Pre (before) vs. Post (after) BAV. Repeat cardiac deviation (SD) is indicated. Notes: Pre: before BAV; Post: after BAV.
catheterization at a mean of 16 months after BAV in 15 patients revealed Reproduced from Rao. 11
an increase (p < 0.01) at intermediate-term follow-up (ITFU). However,
the pressure gradients are lower (p < 0.001) than those before BAV.
Reproduced from Galal et al. 19 5. Late follow-up outcomes
Late follow-up (more than a median or mean of 5 years)
were found to be age under 3 years and post-BAV residual
aortic gradients exceeding 30 mmHg. 18,19 Notably, the outcomes post-BAV have been evaluated by several
66
65
higher the number of risk factors, the greater the probability cardiologists. Hawkins et al., Kuhn et al., and Demkow
67
of obstruction (Figure 16). 18,19 Other investigators studied et al. observed the need for surgical intervention in
63
this issue but could not identify any key factors. The 33% to 45% of patients at long-term follow-up, either to
re-stenosed valve can be successfully balloon dilated by address recurrent AVS or newly developed AI. Reports by
repeat BAV (Figure 17). 64 other investigators were summarized elsewhere. In our
75
Volume 2 Issue 3 (2024) 4 doi: 10.36922/bh.2914