Page 51 - BH-2-3
P. 51
Brain & Heart Balloon valvuloplasty for aortic stenosis
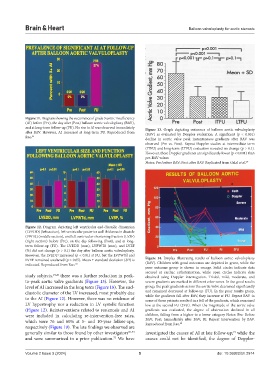
Figure 11. Diagram showing the occurrence of grade 3 aortic insufficiency
(AI) before (Pre), the day after (Post) balloon aortic valvuloplasty (BAV),
and at long-term follow-up (FU). No rise in AI was observed immediately Figure 13. Graph depicting outcomes of balloon aortic valvuloplasty
after BAV. However, AI increased at long-term FU. Reproduced from (BAV) as evaluated by Doppler evaluation. A significant (p < 0.001)
Rao. 11 decline in aortic valve peak instantaneous gradients after BAV was
observed (Pre vs. Post). Repeat Doppler studies at intermediate-term
(ITFU) and long-term (LTFU) evaluation revealed no change (p > 0.1).
However, these Doppler gradients are significantly lower (p < 0.001) than
pre-BAV values
Notes: Pre: before BAV; Post: after BAV. Replicated from Galal et al. 19
Figure 12. Diagram depicting left ventricular end-diastolic dimension
(LVEDD) (left section), left ventricular posterior wall thickness in diastole
(PWTd) (middle section), and left ventricular shortening fraction (LVSF)
(right section) before (Pre), on the day following (Post), and at long-
term follow-up (FU). The LVEDD (mm), LVPWTd (mm), and LVEF
(%) did not change (p > 0.1) the day after balloon aortic valvuloplasty.
However, the LVEDD increased (p < 0.01) at FU, but the LVPWTd and
LVEF remained unaltered (p > 0.05). Mean ± standard deviation (SD) is Figure 14. Display illustrating results of balloon aortic valvuloplasty
indicated. Reproduced from Rao. 20 (BAV). Children with good outcomes are depicted in green, while the
poor outcome group is shown in orange. Solid circles indicate data
secured at cardiac catheterization, while open circles indicate data
study subjects. 19,20 there was a further reduction in peak- obtained using Doppler interrogation. Trivial, mild, moderate, and
to-peak aortic valve gradients (Figure 13). However, the severe gradients are marked in different color zones. In the good results
level of AI increased in the long term (Figure 18). The end- group, the peak gradients across the aortic valve decreased significantly
diastolic diameter of the LV increased, most probably due and remained decreased at follow-up (FU). In the poor results group,
while the gradients fall after BAV, they increase at FU. Repeat BAV in
to the AI (Figure 12). However, there was no evidence of some of these patients resulted in a fall of the gradients, which remained
LV hypertrophy nor a reduction in LV systolic function low at the second FU (2FU). When the magnitude of the aortic valve
(Figure 12). Reinterventions related to restenosis and AI gradients was evaluated, the degree of obstruction declined in all
were included in calculating re-intervention-free rates, children, falling from a higher to a lower category Notes: Pre: Before
which were 76 and 60% at 5- and 10-year follow-ups, BAV; Post: Immediately after BAV; RI: Repeat intervention by BAV.
Reproduced from Rao.
20
respectively (Figure 19). The late findings we observed are
generally similar to those found by other investigators 65-74 investigated the causes of AI at late follow-up; while the
19
and were summarized in a prior publication. We have causes could not be identified, the degree of Doppler-
75
Volume 2 Issue 3 (2024) 5 doi: 10.36922/bh.2914