Page 48 - TD-2-2
P. 48
Tumor Discovery Choroid plexus tumors: Benign to malignant
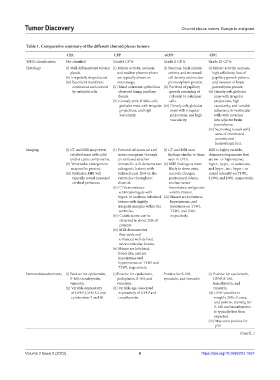
Table 1. Comparative summary of the different choroid plexus tumors
CPA CPP aCPP CPC
WHO classification Not classified Grade I CPTs Grade II CPTs Grade III CPTs
Histology (i) Well-differentiated tubular (i) Mitotic activity, necrosis, (i) Necrosis, brisk mitotic (i) Mitotic activity, necrosis,
glands. and nuclear pleomorphism activity, and increased high cellularity, loss of
(ii) Irregularly shaped acini. are typically absent on cell density and nuclear papillary growth pattern,
(iii) Basement membrane microscopy. pleomorphism present. and invasion of brain
continuous and covered (ii) Bland columnar epithelium (ii) Portions of papillary parenchyma present.
by cuboidal cells. observed lining papillary growth consisting of (ii) Grossly soft, globular
fronds. cuboidal to columnar mass with irregular
(iii) Grossly pink, friable, soft, cells. projections, high
globular mass with irregular (iii) Grossly soft, globular vascularity, and variable
projections, and high mass with irregular adherence to ventricular
vascularity. projections, and high walls with invasion
vascularity. into adjacent brain
parenchyma.
(iii) Sectioning reveals solid
areas of intermixed
necrotic and
hemorrhagic foci.
Imaging (i) CT and MRI may reveal (i) Prenatal ultrasound and (i) CT and MRI scan MRI is highly variable,
calcified mass with solid neurosonogram through findings similar to those demonstrating masses that
and/or cystic components. an unfused anterior seen in CPPs. are iso- or hypointense,
(ii) Ventricular enlargement fontanelle will demonstrate (ii) MRI findings in more hyper-, hypo-, or isointense,
may not be present. echogenic lesions with likely to show cysts, and hypo-, iso-, hyper-, or
(iii) Perfusion MRI will bidirectional flow in the necrotic changes, mixed intensity on T1WI,
typically reveal increased ventricles throughout peritumoral edema, T2WI, and DWI, respectively.
cerebral perfusion. diastole. unclear tumor
(ii) CT demonstrates boundaries, and greater
ventriculomegaly with volume masses.
hyper- to isodense lobulated (iii) Masses are isointense,
lesions with slightly hyperintense, and
irregular margins within the isointense on T1WI,
ventricles. T2WI, and DWI,
(iii) Calcifications can be respectively.
observed in about 25% of
patients.
(iv) MRI demonstrates
flow voids and
enhanced well-defined
intraventricular lesions.
(v) Masses are lobulated,
frond-like, and are
hypointense and
hyperintense on T1WI and
T2WI, respectively.
Immunohistochemistry (i) Positive for cytokeratin, (i)Positive for cytokeratin, Positive for S-100, (i) Positive for cytokeratin,
S-100, transthyretin, podoplanin, S-100, and synuclein, and vimentin. GFAP, S-100,
vimentin. vimentin. transthyretin, and
(ii) Variable expressivity (ii) Variable age-associated vimentin.
of GFAP, CAM 5.2 and expressivity of GFAP and (ii) GFAP positive in
cytokeratins 7 and 20. transthyretin. roughly 20% of cases,
and positive staining for
S-100 and transthyretin
is typically less than
expected.
(iii) May stain positive for
p53.
(Cont’d...)
Volume 2 Issue 2 (2023) 6 https://doi.org/10.36922/td.1057