Page 113 - AN-4-4
P. 113
Advanced Neurology CAA-related inflammatory case
by slow reaction for 2 months, with aggravation and department of our hospital. While waiting for treatment,
abnormal behavior for 1 day.” Two months before seeking the patient developed a disturbance of consciousness
medical consultation, the patient had developed unsteady accompanied by generalized tonic-clonic seizures. He was
walking and a slow reaction without apparent reasons. He admitted to our department for further treatment.
visited the emergency department of our hospital, where a The patient had a history of hypertension and had
cranial computed tomography (CT) scan was conducted, undergone abdominal aortic aneurysm stenting and renal
showing multiple white matter lesions in the brain. When artery stenting. At admission, his body temperature was
he was admitted to the hospital, biochemical tests indicated 36.5°C, pulse rate was 72 beats/min, and blood pressure
that creatinine was 158 μmol/L and serum potassium
was 2.97 mmol/L. The results of blood routine, hepatitis was 166/78 mmHg. The patient was conscious but listless
B, treponema pallidum, human immunodeficiency and was wheeled into the ward on a stretcher. At this point,
virus, and immune tests were normal. Further cranial he had a slow reaction, poor memory of recent events, and
magnetic resonance imaging (MRI) showed multiple old decreased calculation and execution abilities, but normal
hemorrhagic foci in the bilateral frontal lobes, accompanied orientation and remote memory. He became less cooperative
by local brain tissue edema and demyelination, such as during the body examination and was not able to correctly
changes in the white matter of the bilateral occipital lobes respond to all questions asked. At this point, he had a slow
(Figure 1). Total aortic CT angiography indicated severe reaction, poor memory of recent events, and decreased
stenosis of the left renal artery. Cerebrospinal fluid (CSF) calculation and execution abilities, but normal orientation
tests showed that the total protein was 760 mg/L, and the and remote memory. He became less cooperative during
results of CSF biochemistry, routine tests, and tests for the body examination and was not able to correctly respond
autoimmune encephalitis were not significantly abnormal. to all questions asked. The examination of cranial nerves
During hospitalization, the patient’s systolic blood showed no obvious abnormalities. The muscle tone of the
pressure fluctuate around 180 – 200 mmHg, and renal four limbs was normal, the muscle strength of the four limbs
function continued to deteriorate. Creatinine increased was grade 4, and the tendon reflexes of the four limbs were
from 158 μmol/L at admission to 430 μmol/L. The initial symmetrical. The patient was uncooperative during the
diagnosis was reversible posterior leukoencephalopathy examination of deep and superficial sensations, and also
syndrome. Left renal artery stenting was performed. After uncooperative in the finger-nose test and heel-knee-shin test.
the operation, the patient’s blood pressure returned to He was not able to walk in a straight line and cooperate well
normal, and the symptoms of unsteady walking and slow in the Romberg test. The bilateral pathological signs were
reaction improved slightly as compared to the condition at negative, and the meningeal irritation sign was negative.
admission, and then he was discharged. Three weeks after Regarding the laboratory tests and auxiliary
discharge, that is, on July 14, 2023, the patient experienced examinations, his red blood cell count was 2.93 × 10 /L,
12
uncontrolled bowel movement at home in the kitchen high-sensitivity C-reactive protein was 36 mg/L, creatinine
for undetermined reasons. After being discovered by his was 304.3 μmol/L, uric acid was 528.4 μmol/L,
family, the patient was immediately sent to the emergency
potassium was 3.49 mmol/L, albumin was 34.7 g/L,
progastrin-releasing peptide was 132 pg/mL, and the
test results of other tumor markers, rheumatological
and immunological indexes were normal. According
to the lumbar puncture examination, CSF pressure was
150 mmH O, the Pandy test was positive, total CSF
2
protein was 969 mg/L, and the results of other CSF routine
tests, paraneoplastic neurological syndrome antibody
spectrum and metagenomic detection of pathogenic
microorganisms were normal. In cranial MRI, asymmetric
leukoencephalopathy was visible in the whole brain on T2
fluid-attenuated inversion recovery (FLAIR) sequence
(Figure 2A and B), whereas multiple microhemorrhagic
foci were visible on susceptibility-weighted imaging (SWI)
sequence (Figure 3A and B). CT of the chest, abdomen,
and pelvis showed scattered chronic inflammation in
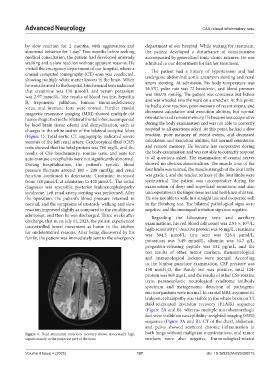
Figure 1. Fluid-attenuated inversion recovery shows abnormally high both lungs without malignant manifestations, and tumor
signals mainly in the posterior part of the brain markers were also negative. Immunological-related
Volume 4 Issue 4 (2025) 107 doi: 10.36922/AN025080015