Page 60 - GTM-2-2
P. 60
Global Translational Medicine New insights into chronic pain management
pathology or distraction. They are the key mechanisms statistically more often in patients with nociceptive pain
that alter the proper functioning of the descending in 82% (Figure 7). Chronic pain is always accompanied
noradrenergic and serotoninergic system . Dysfunction by emotional disorders and insomnia. When the pain
[48]
of the descending noradrenergic and serotoninergic system transforms into chronic pain, a psychological component
is predominant and determines mechanism-oriented comes to the forefront in supporting pain behavior and
treatment . That explains why patients with chronic pain suffering. These results can be explained by the activation
[48]
experienced low efficacy of NSAIDs or anticonvulsants. of nociceptive neurons and certain supraspinal structures,
Antinociceptive activity is regulated by only 5HT1A and such as anterior cingulate cortex, right dorsolateral
5HT2 serotonin receptors, but 5HT3 serotonin receptors prefrontal cortex, left middle frontal gyrus, and left lateral
do not participate in pain control system . Management occipital cortex, as well as PAG region and basal main
[49]
of chronic pain, accompanied by depression, should functions, that are revealed during functional magnetic
include antidepressants that target depression mechanisms resonance imaging. The main functions of these structures
(the main factor of pain chronicity) and chronic pain are to regulate cognition, emotional processes, and
mechanisms. Vortioxetine is an antidepressant with behavior. These interactions provide inseparable affinity
multimode mechanism of action. Vortioxetine acts upon between nociception and patients behavior, including
[12]
5HT1A receptors and 5HT1B receptors, and inhibits 5HT3 mood changes when chronic pain develops . It is known
receptors (Figure 10). that the decrease of serotonin and noradrenaline level
is a key mechanism of depression and antinociceptive
Our data demonstrated pain relief by vortioxetine
treatment in all patient groups regardless of pain origin. dysfunction. Depression does occur significantly more
often in patients with nociceptive pain, and this is a
Patients with neuropathic pain origin had no statistical testament to the significant influence of depression on
difference in pain relief compared with nociceptive pain mechanisms of chronic pain and supporting pain .
[12]
(Table 1). Depression is statistically lower in patients with neuropathic
Most patients had comorbid symptoms: 65% had pain as pronounced neuropathic pain demands intensive
depression and 74% had insomnia. Mood disorders occur attentional resource.
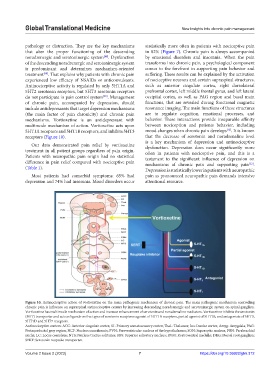
Figure 10. Antinociceptive action of vortioxetine on the main pathogenic mechanism of chronic pain. The main pathogenic mechanism controlling
chronic pain is influence on supraspinal antinociceptive centers by increasing descending noradrenergic and serotoninergic system on spinal ganglion.
Vortioxetine has multimode mechanism of action and increase enhancement of serotonin and noradrenaline mediators. Vortioxetine inhibits the serotonin
(5HT) transporter and acts as ligands on five types of serotonin receptors: agonist of 5HT1A receptors, partial agonist of 5HT1B, and antagonists of 5HT3,
5HT1D and 5HT7 receptors.
Antinociceptive centers: ACC: Anterior cingulate cortex; S1: Primory somatosensory cortex; Thal.: Thalamus; Ins: Insular cortex; Amyg: Amygdala; PAG:
Periaqueductal gray region; NCF: Nucleus cuneiformis; PVN: Paraventricular nucleus of the hypothalamus; SON: Supraoptic nucleus; PBN: Parabrachial
nuclei; LC: Locus coeruleus; NTS: Nucleus tractus solitaries; SSN: Superior salivatory nucleus; RVM: Rostroventral medulla; DRG: Dorsal rout ganglion;
SERT: Serotonin reuptake transporter.
Volume 2 Issue 2 (2023) 7 https://doi.org/10.36922/gtm.312