Page 57 - GTM-2-2
P. 57
Global Translational Medicine New insights into chronic pain management
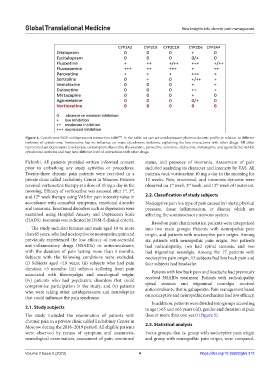
Figure 4. Cytochrome P450 antidepressants interaction table . In the table, we can see antidepressant pharmacokinetic profile in relation to different
[45]
isoforms of cytochrome. Vortioxetine has no influence on main cytochrome isoforms, explaining the low interactions with other drugs. All other
represented antidepressants (citalopram, escitalopram, fluoxetine, fluvoxamine, paroxetine, sertraline, duloxetine, mirtazapine, and agomelatine) inhibit
cytochrome isoforms and may have different level of interactions with other drugs.
Helsinki. All patients provided written informed consent status, and presence of insomnia. Assessment of pain
prior to embarking any study activities or procedures. included analyzing its character and intensity by VAS. All
Twenty-three chronic pain patients were recruited in a patients took vortioxetine 10 mg a day in the morning for
private clinic called Lechebiniy Center in Moscow. Patients 12 weeks. Pain, emotional, and insomnia dynamic were
received vortioxetine therapy at a dose of 10 mg a day in the observed on 1 week, 3 week, and 12 week of treatment.
st
th
rd
morning. Efficacy of vortioxetine was assessed after 1 , 3 ,
st
rd
th
and 12 week therapy using VAS for pain intensity value in 2.2. Classification of study subjects
accordance with comorbid symptoms, emotional disorder Nociceptive pain is a type of pain caused by injury, physical
and insomnia. Emotional disorders such as depression were pressure, tissue inflammation, or disease which are
examined using Hospital Anxiety and Depression Scale affecting the somatosensory nervous system.
(HADS). Insomnia was indicated by DSM-5 clinical criteria.
Based on pain characteristics, patients were categorized
The study included females and male aged 18 to more into two main groups: Patients with neuropathic pain
than 65 years, who had nociceptive or neuropatinc pain and origin, and patients with nociceptive pain origin. Among
previously experienced the low efficacy of non-steroidal six patients with neuropathic pain origin, two patients
anti-inflammatory drugs (NSAIDs) or anticonvulsants, had radiculopathy, two had spinal stenosis, and two
with the duration of pain lasting more than 3 months. had trigeminal neuralgia. Among the 17 patients with
Subjects with the following conditions were excluded: nociceptive pain origin, 13 subjects had low back pain and
(i) Subjects aged <18 years; (ii) subjects who had pain four subjects had headache.
duration <3 months; (iii) subjects suffering from pain
Patients with low back pain and headache had previously
associated with fibromyalgia and oncological origin; received NSAIDs treatment. Patients with radiculopathy,
(iv) patients who had psychiatric disorders that could
compromise participation in the study; and (v) patients spinal stenosis and trigeminal neuralgia received
who were taking other antidepressants and neuroleptics anticonvulsants, that is, gabapentin. Pain management based
that could influence the pain syndrome. on nociceptive and neuropathic mechanism had low efficacy.
In addition, patients were divided into groups according
2.1. Study subjects to age (>65 and ≤65 years old), gender and duration of pain
The study included the examination of patients with (less or more than one year) (Figure 5).
chronic pain in a private clinic called Lechebiniy Center in
Moscow during the 2018–2019 period. All eligible patients 2.3. Statistical analysis
were observed by means of symptom and anamnesis, Focus groups, that is, group with nociceptive pain origin
neurological examination, assessment of pain, emotional and group with neuropathic pain origin, were compared.
Volume 2 Issue 2 (2023) 4 https://doi.org/10.36922/gtm.312