Page 123 - MI-1-1
P. 123
Microbes & Immunity Rare multi-site Klebsiella pneumoniae infections
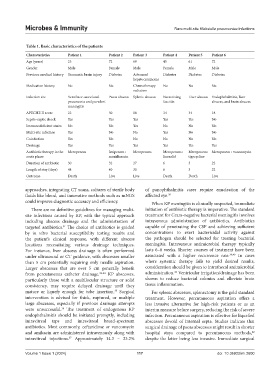
Table 1. Basic characteristics of the patients
Characteristics Patient 1 Patient 2 Patient 3 Patient 4 Patient 5 Patient 6
Age (years) 23 72 69 45 61 72
Gender Male Female Male Female Male Male
Previous medical history Traumatic brain injury Diabetes Advanced Diabetes Diabetes Diabetes
hepatocarcinoma
Medication history No No Chemotherapy No No No
radiation
Infection site Ventilator-associated Psoas abscess Splenic abscess Necrotizing Liver abscess Endophthalmitis, liver
pneumonia and purulent fasciitis abscess, and brain abscess
meningitis
APECHE II score 23 30 18 34 34 18
Sepsis–septic shock Yes Yes Yes Yes Yes No
Immunodeficient states No No Yes No No No
Multi-site infection Yes No No Yes No No
Coinfection Yes No No No No No
Drainage Yes Yes Yes Yes Yes Yes
Antibiotic therapy in the Meropenem Imipenem+ Meropenem Meropenem+ Meropenem+ Meropenem+ vancomycin
acute phase moxifloxacin linezolid tigecycline
Duration of antibiotic 30 32 27 6 3 22
Length of stay (days) 44 40 30 6 3 22
Outcome Death Live Live Death Death Live
approaches, integrating CT scans, cultures of sterile body of panophthalmitis cases require enucleation of the
fluids like blood, and innovative methods such as mNGS affected eye. 38
could improve diagnostic accuracy and efficiency. When KP meningitis is clinically suspected, immediate
There are no definitive guidelines for managing multi- initiation of antibiotic therapy is imperative. The standard
site infections caused by KP, with the typical approach treatment for Gram-negative bacterial meningitis involves
including abscess drainage and the administration of intravenous administration of antibiotics. Antibiotics
targeted antibiotics. The choice of antibiotics is guided capable of penetrating the CSF and achieving sufficient
31
by in vitro bacterial susceptibility testing results and concentrations to exert bactericidal activity against
the patient’s clinical response, with different abscess the pathogen should be selected for treating bacterial
locations necessitating various drainage techniques. meningitis. Intravenous antimicrobial therapy typically
For instance, liver abscess drainage is often performed lasts 6–8 weeks. Shorter courses of treatment have been
under ultrasound or CT guidance, with abscesses smaller associated with a higher recurrence rate. 39,40 In cases
than 5 cm potentially requiring only needle aspiration. where systemic therapy fails to yield desired results,
Larger abscesses that are over 5 cm generally benefit consideration should be given to intrathecal antimicrobial
41
from percutaneous catheter drainage. 32-34 KP abscesses, administration. Ventricular irrigation/drainage has been
particularly those with a multilocular structure or solid shown to reduce bacterial colonies and alleviate brain
consistency, may require delayed drainage until they tissue inflammation.
mature or liquefy enough for tube insertion. Surgical For splenic abscesses, splenectomy is the gold standard
35
intervention is advised for thick, ruptured, or multiple treatment. However, percutaneous aspiration offers a
large abscesses, especially if previous drainage attempts less invasive alternative for high-risk patients or as an
36
were unsuccessful. The treatment of endogenous KP interim measure before surgery, reducing the risk of severe
endophthalmitis should be initiated promptly, including infection. Percutaneous aspiration is effective for liquefied
intravitreal taps and intravitreal broad-spectrum abscesses devoid of internal septa. Studies indicate that
antibiotics. Most commonly, ceftazidime or vancomycin surgical drainage of psoas abscesses might result in shorter
and amikacin are administered intravenously along with hospital stays compared to percutaneous methods,
42
intravitreal injections. Approximately 14.3 – 23.2% despite the latter being less invasive. Immediate surgical
37
Volume 1 Issue 1 (2024) 117 doi: 10.36922/mi.2600