Page 71 - TD-2-2
P. 71
Tumor Discovery SRT with SIP planning for synovial sarcoma
A B
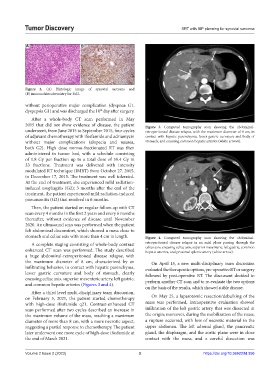
Figure 2. (A) Histologic image of synovial sarcoma and
(B) immunohistochemistry for Bcl2.
without perioperative major complication (dyspnea G1,
dyspepsia G1) and was discharged the 10 day after surgery.
th
After a whole-body CT scan performed in May
2015 that did not show evidence of disease, the patient Figure 3. Computed tomography scan showing the abdominal-
underwent, from June 2015 to September 2015, four cycles retroperitoneal disease relapse, with the maximum diameter of 8 cm, in
of adjuvant chemotherapy with ifosfamide and adriamycin contact with hepatic parenchyma, lesser gastric curvature and body of
without major complications (alopecia and nausea, stomach, and encasing common hepatic arteries (white arrows).
both G2). High dose normo-fractionated RT was then
administered to tumor bed, with a schedule consisting
of 1.8 Gy per fraction up to a total dose of 59.4 Gy in
33 fractions. Treatment was delivered with intensity
modulated RT technique (IMRT) from October 27, 2015,
to December 17, 2015. The treatment was well tolerated.
At the end of treatment, she experienced mild radiation-
induced esophagitis (G2); 3 months after the end of the
treatment, the patient experienced mild radiation-induced
pneumonitis (G2) that resolved in 6 months.
Then, the patient started on regular follow-up with CT
scan every 4 months in the first 2 years and every 6 months
thereafter, without evidence of disease until November
2020. An ultrasound scan was performed when the patient
felt abdominal discomfort, which showed a mass close to
stomach and celiac axis with more than 4 cm in length. Figure 4. Computed tomography scan showing the abdominal-
A complete staging consisting of whole-body contrast retroperitoneal disease relapse in an axial plane passing through the
enhanced CT scan was performed. The study described celiax axis, encasing celiac axis, superior mesenteric, left gastric, common
hepatic arteries, and proximal splenic artery (white arrow).
a huge abdominal-retroperitoneal disease relapse, with
the maximum diameter of 8 cm, characterized by an On April 15, a new multi-disciplinary team discussion
infiltrating behavior, in contact with hepatic parenchyma, evaluated the therapeutic options, pre-operative RT or surgery
lesser gastric curvature and body of stomach, clearly followed by post-operative RT. The discussant decided to
encasing celiac axis, superior mesenteric artery, left gastric, perform another CT scan and to re-evaluate the two options
and common hepatic arteries (Figures 3 and 4).
on the basis of the results, which showed stable disease.
After a third level multi-disciplinary team discussion,
on February 5, 2021, the patient started chemotherapy On May 25, a laparotomic resection/debulking of the
with high-dose ifosfamide q21. Contrast-enhanced CT mass was performed, intraoperative evaluation showed
scan performed after two cycles described an increase in infiltration of the left gastric artery that was dissected at
the maximum volume of the mass, reaching a maximum the origin; moreover, during the mobilization of the mass,
diameter of more than 8 cm, with a more necrotic aspect, a rupture occurred, with loss of necrotic material in the
suggesting a partial response to chemotherapy. The patient upper abdomen. The left adrenal gland, the pancreatic
later underwent one more cycle of high-dose ifosfamide at gland, the diaphragm, and the aortic plane were in close
the end of March 2021. contact with the mass, and a careful dissection was
Volume 2 Issue 2 (2023) 3 https://doi.org/10.36922/td.356