Page 58 - ARNM-1-1
P. 58
Advances in Radiotherapy
& Nuclear Medicine Refractory pulmonary adenocarcinoma
A
B E H
C F I
D G J
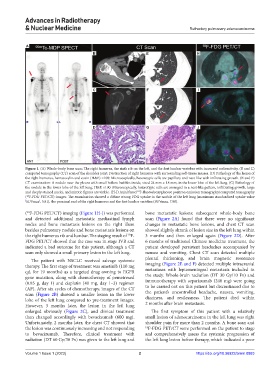
Figure 1. (A) Whole-body bone scan: The right humerus, the sixth rib on the left, and the first lumbar vertebra with increased radioactivity. (B and C)
computed tomography (CT) scan of the shoulder joint: Destruction of right humerus with surrounding soft-tissue masses. (D) Pathology of the lesion of
the right humerus, hematoxylin and eosin (H&E) ×100: Microscopically, heterotypic cells are papillary and nest-like with infiltrating growth. (E and F)
CT examination: A nodule near the pleura with small hollow bubbles inside, sized 24 mm × 18 mm, in the lower lobe of the left lung. (G) Pathology of
the nodule in the lower lobe of the left lung, H&E ×100: Microscopically, heterotypic cells are arranged in a nest-like pattern, infiltrating growth, large
18
and deeply stained nuclei, and mitotic figures are visible. (H-J) Axial fused F-fluorodeoxyglucose positron emission tomography/computed tomography
( F-FDG PET/CT) images: The examination showed a diffuse strong FDG uptake in the nodule of the left lung (maximum standardized uptake value
18
]
[ SUVmax , 5.81), the proximal end of the right humerus and the first lumbar vertebra (SUVmax, 7.98).
( F-FDG PET/CT) imaging (Figure 1H-J) was performed bone metastatic lesions; subsequent whole-body bone
18
and detected additional metastatic mediastinal lymph scan (Figure 2A) found that there were no significant
nodes and bone metastasis lesions on the right illum changes in metastatic bone lesions, and chest CT scan
besides pulmonary nodule and bone metastasis lesions on showed slightly shrank of lesion size in the left lung within
the right humerus rib and lumbar. The staging result of F- 3 months and then enlarged again (Figure 2D). After
18
FDG PET/CT showed that the case was in stage IVB and 6 months of traditional Chinese medicine treatment, the
indicated a bad outcome for this patient, although a CT patient developed persistent headaches accompanied by
scan only showed a small primary lesion in the left lung. nausea and vomiting. Chest CT scan detected multiple
The patient with NSCLC received salvage systemic pleural thickening, and brain magnetic resonance
therapy. The first stage of treatment was ametinib (110 mg imaging (Figure 2E and F) detected multiple intracranial
qd, for 19 months) as a targeted drug owning to EGFR metastases with leptomeningeal metastasis included in
gene mutation, along with chemotherapy of pemetrexed the study. Whole-brain radiation (DT 30 Gy/10 Fx) and
(0.85 g, day 1) and cisplatin (40 mg, day 1–3) regimen immunotherapy with separizumab (240 mg) were going
(AP). After six cycles of chemotherapy, images of the CT to be carried out on this patient but discontinued due to
scan (Figure 2B) showed a smaller lesion in the lower the patient’s uncontrolled headache, nausea, vomiting,
lobe of the left lung compared to pre-treatment images. dizziness, and restlessness. The patient died within
However, 3 months later, the lesion in the left lung 2 months after brain metastasis.
enlarged obviously (Figure 2C), and clinical treatment The first symptom of this patient with a relatively
then changed accordingly with bevacizumab (600 mg). small lesion of adenocarcinoma in the left lung was right
Unfortunately, 2 months later, the chest CT showed that shoulder pain for more than 2 months. A bone scan and
the lesion was continuously increasing and not responding 18 F-FDG PET/CT were performed on the patient to stage
to bevacizumab. Therefore, clinical treatment with and comprehensively assess the systemic progression of
radiation (DT 60 Gy/30 Fx) was given to the left lung and the left lung lesion before therapy, which indicated a poor
Volume 1 Issue 1 (2023) 2 https://doi.org/10.36922/arnm.0883